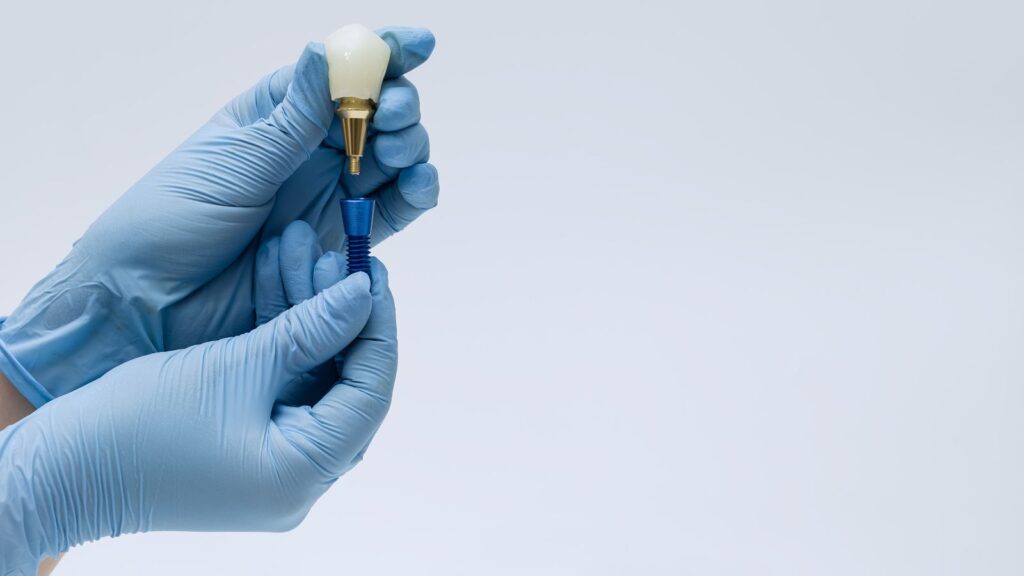
Choosing between titanium and zirconia implants affects how your restored tooth looks, feels, and integrates with your jawbone. Titanium has a long clinical track record with excellent strength and durability, while zirconia offers a metal-free alternative with a more natural, tooth-colored appearance that appeals to some patients.
This guide provides a clear comparison of each material’s performance in durability, biocompatibility, and aesthetics. You’ll also learn the practical considerations your dentist evaluates—such as bite force, gum thickness, medical history, and long-term maintenance—when recommending one option over the other. With straightforward explanations of implant design and treatment steps, you’ll be better prepared to make an informed decision. For personalized guidance based on your goals and oral health, consulting Renaissance Dental Implant Center in New Orleans, LA can help you determine which material best fits your needs.
Overview of Dental Implant Materials
Different implant materials affect strength, appearance, and tissue response. Choosing the right material changes how your implant integrates, looks in the mouth, and performs under bite forces.
Importance of Material Choice
Your material choice influences long-term success, aesthetic outcome, and risk of complications. Titanium has decades of clinical data showing high osseointegration rates under load, while zirconia offers a tooth-colored option that reduces visible metal in thin tissue biotypes.
Consider patient-specific factors: smoking, bruxism, allergy history, and thin gingival biotype all shift the risk–benefit balance. For example, heavy grinders may favor titanium alloys for fatigue resistance; patients with metal sensitivity or high aesthetic demands may prefer zirconia.
Costs and restorative workflow matter too. Titanium systems provide wide implant and prosthetic options, often lowering cost and simplifying restorative stages. Zirconia implant options are expanding but still have fewer size and connection choices, which can affect treatment planning and lab work.
Common Materials Used in Dental Implants
Primary materials: titanium (commercially pure Ti and Ti-6Al-4V alloy) and zirconia (yttria-stabilized tetragonal zirconia polycrystal, Y-TZP).
Titanium: strong, ductile, and well-documented for osseointegration. Manufacturers use surface treatments (acid-etching, grit-blasting, anodization) to increase bone contact and accelerate healing. Ti-6Al-4V improves strength for narrow-diameter applications.
Zirconia: a high-strength ceramic with favorable aesthetics and low plaque affinity. Most zirconia implants are one-piece or limited two-piece designs; newer two-piece systems are emerging but remain less common.
Hybrid designs also exist: titanium cores with zirconia abutments combine strength and tooth-colored transmucosal components.
Other materials: PEEK and polymer composites appear in experimental or provisional roles but lack long-term evidence for definitive implant posts.
Material Properties and Biocompatibility
Mechanical properties: titanium exhibits high tensile strength and fatigue resistance; zirconia shows high compressive strength but lower toughness and different fracture behavior. That affects implant diameter selection and restoration design.
Biocompatibility: titanium demonstrates predictable bone apposition and immune tolerance in most patients. Rare metal hypersensitivity reports exist; patch testing can guide decisions when you suspect allergy.
Zirconia shows low ion release and favorable soft-tissue response, often with reduced mucosal discoloration. Soft-tissue attachment and lower bacterial adhesion in some studies may benefit peri-implant health.
Surface chemistry and topography drive cellular responses. Both materials rely on optimized surfaces to promote osteoblast attachment; differences in surface processing alter healing timelines and primary stability.
Titanium Dental Implants
Titanium implants are the most widely used implant material and are known for their strength, proven long-term success, and versatility across clinical situations. You will most often encounter titanium implants when your dentist needs reliable osseointegration, customizable shapes, and restorative flexibility.
Key Characteristics of Titanium
- Material type: Commercially pure titanium or titanium alloys (commonly Ti-6Al-4V).
- Osseointegration: Titanium forms a direct bone-to-implant interface. This biological bonding reduces micro-movement and supports long-term stability.
- Mechanical properties: High tensile strength and fatigue resistance allow thin implant walls and varied designs (root-form, tapered, short, narrow).
- Surface treatments: Roughening, plasma-spraying, acid-etching, or anodization are common to increase surface area and speed bone attachment.
- Radiopacity: Titanium shows clearly on X-rays, helping you and your clinician assess integration and detect complications.
- Corrosion resistance: Forms a passive oxide layer that protects against degradation in the oral environment.
Advantages of Titanium Implants
- High success rates: Large clinical datasets show predictable outcomes across single-tooth, multiple, and full-arch restorations.
- Design flexibility: You can choose from many implant geometries, lengths, and diameters to match bone volume and prosthetic needs.
- Restorative compatibility: Widely compatible with stock and custom abutments, CAD/CAM workflows, and screw- or cement-retained prostheses.
- Bone preservation: Strong primary stability supports immediate or early loading protocols in appropriate cases.
- Cost and availability: Generally less expensive and more available than zirconia, with many manufacturers and proven components.
- Long-term data: Decades of follow-up studies inform risk profiles and maintenance guidelines.
Potential Limitations and Considerations
- Aesthetics in thin gingiva: Titanium may show a grayish hue under thin soft tissue or in the esthetic zone, potentially affecting final appearance.
- Allergy and sensitivity: True titanium allergy is rare, but documented hypersensitivity or adverse soft-tissue responses can occur; investigate suspected reactions with medical history and testing.
- Peri-implantitis risk: Like all implants, titanium implants can develop peri-implant mucositis or peri-implantitis; plaque control and regular recall reduce risk.
- Surface wear and microgaps: Micro-movements at implant–abutment connections can harbor bacteria; proper connection choice and maintenance matter.
- Imaging artifacts with CBCT/MRI: Titanium produces minimal CT artifacts but can affect MRI sequences; discuss imaging needs with your clinician.
- Patient factors: Smoking, uncontrolled diabetes, and poor bone quality negatively affect outcomes; your clinician will evaluate systemic and local risks before placement.
Zirconia Dental Implants
Zirconia implants are ceramic fixtures made from zirconium dioxide that emphasize aesthetics, biocompatibility, and a metal-free option for tooth replacement. You’ll find they differ from titanium in composition, surface treatment, and clinical handling.
Features and Composition of Zirconia
Zirconia (zirconium dioxide, ZrO2) is a high-strength ceramic stabilized with yttria to improve fracture toughness. Manufacturers form implants by sintering then machining or using one-piece and two-piece designs; many clinical systems use a one-piece form to avoid microgaps.
Surface modification—such as sandblasting, acid etching, or laser texturing—aims to improve bone integration by increasing surface roughness and wettability.
Zirconia shows low electrical conductivity and no galvanic corrosion, which matters if you have metal sensitivities or multiple metal restorations. It’s white in color, helping mask dark gingival tissue and improving final crown translucency where aesthetics matter.
Benefits of Zirconia Implants
You benefit from a tooth-colored implant body that reduces gray show-through at the gumline, especially with thin gingival biotypes.
Ceramic’s biocompatibility correlates with low inflammatory response in many studies; soft tissue often adheres well to zirconia surfaces, which can help with a stable peri-implant mucosal seal.
If you prefer a metal-free restoration for personal or allergy reasons, zirconia eliminates titanium exposure.
Zirconia resists corrosion and plaque accumulation reasonably well; these properties can support longer-term peri-implant tissue health when combined with good oral hygiene.
Possible Drawbacks and Challenges
Zirconia is ceramics-based and can have lower fracture toughness than titanium alloys, especially in narrow-diameter or long-span implant designs. You should avoid placing single-piece zirconia implants where high lateral forces are expected.
Fewer long-term outcome studies and limited variety of prosthetic components exist compared with titanium systems, so restorative options and clinical protocols may be more constrained.
Occlusal load management and precise surgical placement are critical because repair or modification of zirconia implants is difficult; intraoral adjustments risk microcracks.
Finally, some surface treatments and two-piece zirconia systems are evolving; discuss system-specific evidence and clinician experience with your dentist before choosing zirconia.
Choosing Between Titanium and Zirconia Implants
You’ll weigh strength, appearance, health factors, and your dentist’s clinical judgment when choosing between titanium and zirconia. Cost, long-term data, and the location of the missing tooth also play important roles in the decision.
Comparative Analysis of Performance
Titanium implants show decades of clinical success and a high long-term survival rate in posterior and full-arch restorations. The titanium alloy’s strength and slight flexibility help absorb occlusal forces, reducing fracture risk under heavy chewing loads.
Zirconia implants offer good short- to mid-term success but have less long-term data than titanium, especially for multi-unit or posterior load-bearing cases. Zirconia is more brittle; clinicians may avoid it when you need multi-implant bridges or when bone support is limited.
Consider bone quality and the restoration type: choose titanium for predictability with molars and full-arch work; consider zirconia for single anterior teeth or when you require a metal-free option and have favorable bone conditions.
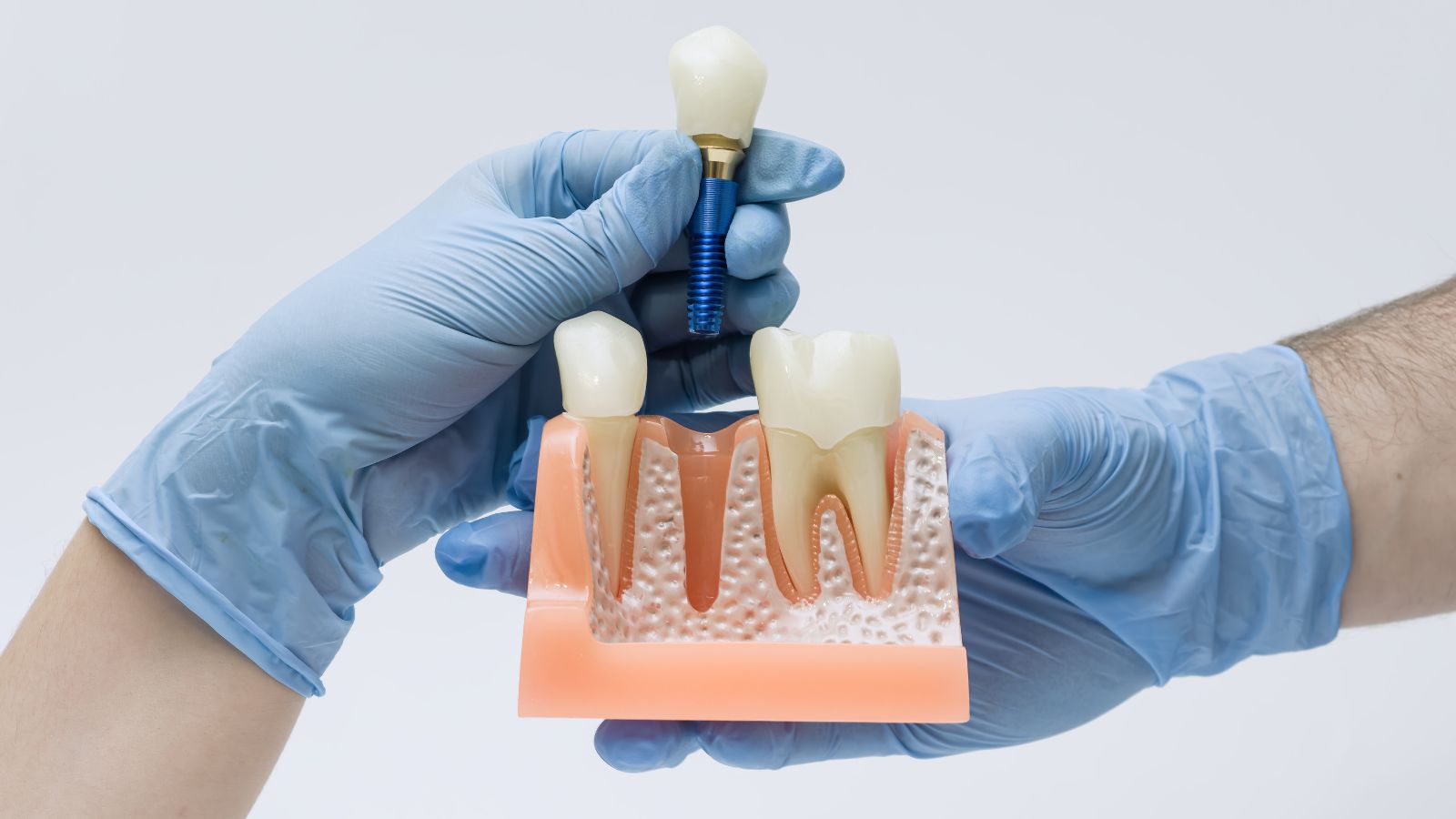
Aesthetic Results and Suitability
Zirconia’s tooth-colored material prevents gray show-through and can give more natural gingival appearance, especially if you have thin gum tissue or a high smile line. This makes zirconia attractive for front-tooth restorations where you want minimal metal visibility.
Titanium can cause a grayish hue at the gum margin if soft tissue is thin or recedes. You can mitigate this with careful implant positioning, thicker soft tissue grafting, or titanium implants with restorative components that mask color.
If your priority is a highly esthetic single anterior tooth and you have healthy gingiva, zirconia often delivers the best visual outcome. For posterior teeth where aesthetics matter less, titanium typically remains the preferred choice.
Patient Health and Allergies
Most patients tolerate titanium well; true titanium allergy is rare. If you have a documented metal hypersensitivity or systemic reaction history, discuss patch testing or consultation with an allergist before implant selection.
Zirconia offers a metal-free alternative and may reduce concerns about galvanic reactions or suspected metal sensitivities. It also shows favorable soft-tissue response and low plaque accumulation in some studies.
If you have autoimmune disease, a history of peri-implantitis, or heightened sensitivity concerns, work closely with your dentist to review medical records and consider material choice alongside infection-control and maintenance plans.
Clinical Recommendations
Your clinician will assess jawbone volume, occlusion, parafunctional habits (e.g., bruxism), and the planned prosthesis before recommending a material. Expect titanium to be suggested for multi-unit prostheses, immediate loading in dense bone, or where long-term evidence is paramount.
Expect zirconia to be recommended for single-tooth anterior replacements, patients seeking metal-free options, and cases with excellent bone and soft-tissue conditions. Some clinicians use a hybrid approach: titanium root with zirconia abutment or crown to balance strength and esthetics.
Discuss costs, expected lifespan, and required maintenance with your dentist. Ask about their experience with each material, relevant case studies, and the specific implant system they plan to use so you can make an informed decision.