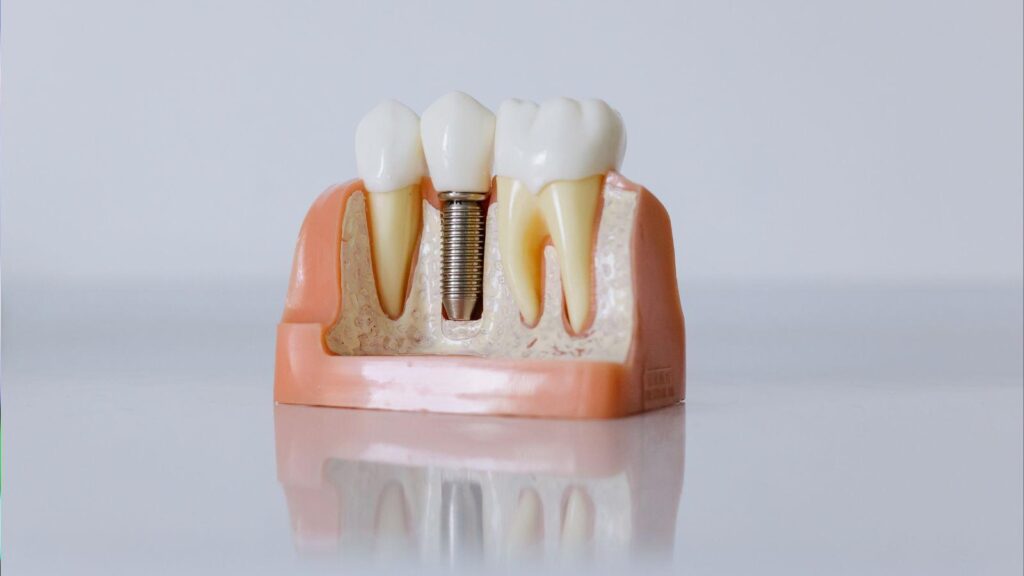
You can get basic stability with just two implants for a lower denture, especially if your jaw bone and oral health are suitable. Two implants act like anchors that stop the denture from slipping, giving you better chewing and more confidence than traditional dentures — all achievable with implant supported dentures in Easton, PA.
You will want to know how your bone quality, mouth shape, and lifestyle affect success, and how prosthetic design and materials change comfort and function. Keep reading to learn when two implants are enough, when more may help, and what your dentist will evaluate before recommending the best option for your situation.
Principles of Implant-Supported Denture Stability
You need a clear grasp of what keeps an implant-supported denture stable: how retention differs from stability, how two implants handle forces, and how your jaw bone and soft tissues affect outcomes.
Defining Denture Retention and Stability
Retention means how well the denture resists vertical movement—how hard it is to pull the denture away from your mouth. Attachments like ball, locator, or bar systems create that vertical hold. Retention also depends on how well the denture base fits the soft tissues and on the seal with saliva and mucosa.
Stability means resistance to horizontal or rotational movement during chewing and speaking. Two implants can control rotation if they sit far enough apart and use the right attachment type. You should know that good retention alone doesn’t prevent tipping; both retention and stability matter for function and comfort.
Key practical points:
- Attachment choice affects both retention and allowed rotation.
- Precise implant placement and denture fit reduce sore spots.
- Maintenance of attachments (replacement every few years) preserves function.
Biomechanics of Two-Implant Solutions
Two implants in the lower jaw usually sit in the canine or lateral incisor positions. This placement balances forces across the denture and limits rotational movement around a midline axis. When you bite, loads transfer from the denture to the implants and the mucosa; implants take vertical loads while the ridge shares horizontal and distributed forces.
Attachment type changes biomechanics:
- Ball/locator: allows some rotation, easier cleaning.
- Bar: links implants to reduce movement, needs more space.
- Fixed hybrid on two implants is rare; usually needs more implants.
Spacing and parallelism matter. Wider implant spacing increases leverage against tipping. Slight implant angulation can be tolerated with angled abutments, but too much torque raises failure risk.
Role of Jaw Anatomy in Treatment Success
Your bone volume and density determine primary implant stability. Dense bone in the anterior mandible gives better initial fixation for two-implant overdentures. Thin or resorbed ridges reduce implant options and may require bone grafts or additional implants.
Soft tissue height and tongue space affect denture extension and attachment choice. A high lingual frenum or shallow vestibule can destabilize the denture or limit attachment selection. Saliva quality and ridge shape influence suction and comfort.
Assess these factors before planning:
- Bone height and width (CBCT helps measure).
- Ridge shape and mucosal thickness.
- Occlusion and parafunctional habits like grinding.
Clinical Case Selection and Assessment
You need to confirm the patient can tolerate two implants, has realistic expectations, and presents anatomy that allows predictable implant placement and overdenture retention.
Patient Suitability Criteria
You should assess medical and dental history for conditions that affect healing or implant success. Look for uncontrolled diabetes, recent bisphosphonate use, head and neck radiotherapy, or heavy smoking; these raise risk and may require medical clearance or altered plans.
Evaluate oral health: active periodontal disease, untreated caries, or poor oral hygiene must be managed before implant surgery. Check mucosal health and denture-bearing tissue for irritation or pathology.
Consider function and expectations. Confirm the patient wants improved retention and understands maintenance needs, follow-up visits, and possible relines. Age alone is not a contraindication; focus on functional needs, manual dexterity, and cognitive ability to manage hygiene.
Diagnostic Imaging and Planning
Obtain a CBCT scan to measure ridge height, width, and the location of the inferior alveolar nerve and mental foramina. Use cross-sectional views to identify areas with 6–8 mm bone height and at least 5 mm width for predictable implant placement.
Take diagnostic casts and a new or well-fitting record denture to record vertical dimension and occlusal plane. Use dual-scan or radiographic stent techniques when anatomy is borderline to plan implant position relative to prosthetic teeth.
Plan implant length and diameter based on available bone and prosthetic load. Choose attachment type (ball, locator, bar) after locating implant sites; plan for 20–30 degrees angulation correction if needed. Document soft tissue thickness for cuff height and healing protocol.
Managing Anatomical Limitations
When ridge height or width is limited, consider short or narrow implants only after confirming primary stability >= 35 Ncm for immediate loading. If primary stability is low, stage placement and allow submerged healing.
For atrophic mandibles near the mental foramen, shift implants slightly anterior to the foramen or use angled placement to avoid nerve injury. Consider ridge augmentation, guided bone regeneration, or onlay grafts when space allows and the patient accepts added cost and time.
If the maxilla opposes the arch, assess interocclusal space. Plan teeth setup and possible prosthetic vertical increase rather than extensive bone grafting. Use reduced-profile attachments when space is limited to preserve denture thickness and strength.
Prosthetic Design and Material Choices
You will decide on attachments that control retention and stability, choose materials that resist wear and fracture, and plan for simple maintenance and repairs. Each choice affects fit, patient comfort, cost, and long-term function.
Implant Attachment Systems Overview
Choose attachment systems based on the retention you need and the space available. Common options include bar, ball (stud), locator/stud, and magnetic attachments. Bars give strong cross-arch support but need more vertical and horizontal space. Studs and locators take less space and are easier to clean and repair.
Match attachment type to jaw anatomy and patient ability. For patients with limited dexterity, low-profile locators or resilient studs reduce insertion force. If you expect heavy chewing forces, consider a bar or splinted solution to spread load across implants.
Consider maintenance needs when you choose. Replace worn nylon inserts on locator systems regularly. Magnets corrode less but can lose retention and are less common for high-function needs. Document planned replacement intervals for inserts, O-rings, or clips.
Material Options for Longevity
Pick denture base and tooth materials for strength and wear resistance. Common base choices are acrylic (PMMA) and metal-reinforced frameworks. PMMA is easy to adjust and repair; metal frameworks add rigidity and reduce fracture risk when space allows.
For denture teeth, choose composite or acrylic teeth for ease of repair and shock absorption, or ceramic for higher wear resistance where occlusion is stable. Hybrid designs—acrylic teeth on metal or reinforced bases—balance aesthetics and durability.
Consider implant component materials too. Titanium implants and attachments provide proven strength and biocompatibility. Avoid mismatched metals when possible to reduce corrosion risk. Always factor in expected bite forces, bruxism, and opposing dentition when selecting materials.
Regular Maintenance and Aftercare
Schedule check-ups at predictable intervals: initial follow-up at 1–2 weeks, then at 6 months, and annually or more often if problems arise. At appointments, assess attachment wear, prosthesis fit, tissue health, and occlusion.
Teach the patient daily cleaning: remove the denture (if removable), rinse, brush attachments gently, and soak according to manufacturer guidance. Replace worn inserts, O-rings, or clips when retention drops or at recommended intervals—often every 6–18 months depending on use.
Keep simple repair tools and replacement parts on hand. Quick in-office swaps of nylon inserts or relines prevent failure and improve patient satisfaction. Document each maintenance visit and any part replacements for future planning.